Dysphagia
Dysphagia is the term used to describe difficulty in swallowing whether it is temporary or permanent.
Dysphagia is not usually classed as a disease itself, but a side-effect of a variety of conditions and can affect a person for any number of medical reasons. When Alex was diagnosed with his condition and we started to find out about dysphagia, we were not aware, then, as to how many people are affected by it or what conditions caused it. Therefore, I list some instances below, in no particular order. However, if you are reading this guide and suffer from dysphagia, you must remember that it DOES NOT MEAN THAT YOU ARE SUFFERING FROM ANY OTHER CONDITION LISTED HERE EXCEPT THE ONE WITH WHICH YOU HAVE BEEN DIAGNOSED.
Occurrence
- Progressive neurodegenerative diseases such as
- Multiple Sclerosis (MS)
- Amyotrophic Lateral Sclerosis (ALS)
- Motor Neurone Disease (MND)
- Parkinson's disease
- Alzheimer's
- Non-progressive motor diseases such as
- Cerebral Palsy
- Other conditions such as
- Autoimmune diseases
- Inflammatory muscle conditions of the oesophagus such as myositis
- If the oesophagus itself becomes deformed or narrowed due to
- A tumour
- Scar tissue forming after radiotherapy in the oesophageal area
- Scar tissue forming from chronic acid reflux
- It also can affect young children - those with
- Cerebral palsy
- Head traumas
- Neurological problems with which they are born
- Some breathing problems such as
- Asthma
- Chronic obstructive pulmonary disease (COPD)
- It can also occur in people who have had
- A stroke
- A brain tumour
Dysphagia is particularly common among older people, as ageing can lead to weakened jaw muscles, loss of teeth and reduced saliva production which are all part of the swallowing and digestion process. Since older people are also more likely to suffer with conditions like dementia, MND, Parkinson’s disease, Alzheimer’s etc, so dysphagia becomes more common in the elderly.
The above list is by no means exhaustive. However, dysphagia is a common problem affecting people of all ages with assorted conditions and it can be progressive, stable, permanent or temporary depending on the condition.
Symptoms
These can range from discomfort when swallowing to actually losing the ability to swallow. These include (depending on the condition):
- inability to control food or saliva in the mouth
- difficulty initiating a swallow
- coughing
- choking
- frequent chest infections
- unexplained weight loss
- pain when swallowing
- gurgly or wet voice after swallowing
- feeling that food is stuck in the oesophagus
- regurgitation when food gets stuck in the oesophagus
Treatment
It may be suggested that you meet with a Speech and Language Therapist which may sound a little strange. (I know we found it odd at first!) However, these therapists are trained to advise on dysphagia and diet and may offer possible exercises to improve swallowing. So do take up the offer if it is made as some types of dysphagia can (sometimes) be partly treated by rehabilitative exercises of the mouth, tongue etc.
Most forms of dysphagia, however, need a change to the texture and consistency of food as it is important to avoid choking and aspiration. Aspiration occurs when food or drink is inhaled into the lungs via the trachea (windpipe) instead of going down into the stomach via the oesophagus. The hinged trapdoor over the trachea does not do its job!
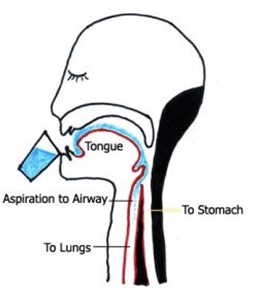
Going down the wrong way – to be avoided!
This can lead to aspiration pneumonia and generally needs to be treated in hospital as it often accompanies a chest infection.
Some dysphagic patients can eat food of relatively any consistency, but only have problems with liquids (see Viscosity section below). This can be easily remedied by using thickeners recommended by your medical professional / dietician. For people with severe dysphagia, the diet changes may mean consuming puréed food.
People with a narrowed oesophagus can sometimes undergo an oesophageal dilation (gullet stretch) or even have a stent (tube) inserted into the oesophagus to widen it so that food can pass more easily into the stomach.
Either way, irrespective as to cause or condition, aspiration is to be avoided at all costs. Food and drink do not belong in the lungs! Any treatment prescribed will have aspiration avoidance as the prime aim.
In rare and extreme cases of dysphagia, if a patient cannot swallow anything at all for whatever reason or the choking hazard becomes too great a risk, a PEG (or "G") feeding tube may then be considered so as to avoid malnutrition. This is where a special tube is inserted through the stomach wall into the stomach so food is no longer taken orally. This is generally regarded as a long-term treatment.